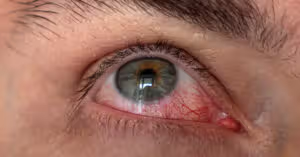
A practical guide from a Calgary optometry team — for the patients who’ve tried artificial tears for months without lasting relief.
Calgary has one of the driest urban climates in Canada. Average relative humidity runs in the thirties through winter, drops further during Chinook events, and rarely exceeds fifty percent even in summer. Combine that with the elevation (1,045 metres above sea level), the forced-air heating that every Alberta home runs for eight months a year, and the average Calgarian’s seven-to-nine hours of daily screen time, and the result is a city that manufactures dry eye disease on an industrial scale.
Most Calgary adults experience dry-eye symptoms at some point; a meaningful minority — one in four by some optometric estimates — carry the clinical form. Artificial tears blunt the worst of it for a few hours. What they don’t do is address the underlying problem, which is almost never a simple shortage of tears. This is a contractor-style look at what dry eye actually is, why Calgary is worse than almost anywhere else in the country, and what a structured treatment plan looks like when drops have stopped working.
Dry eye is rarely a shortage of water
The tear film has three layers. The innermost is mucin, which holds the tear to the eye surface. The middle layer is aqueous, the watery component that most people think of as ‘tears.’ The outer layer is an oil film — the lipid layer — secreted by meibomian glands along the inner edge of each eyelid. That oil layer is what prevents the watery component underneath from evaporating.
Evaporative dry eye, driven by a deficient lipid layer, accounts for roughly 80 percent of all dry-eye cases. The aqueous-deficient form — where the eye simply doesn’t produce enough water — accounts for a much smaller share. Yet almost every patient who walks into a pharmacy for the first time is sold a product that adds water. It is the wrong intervention for four out of five patients.
This is why dry eye so often ‘stops responding’ to artificial tears after a few months. The drops were never fixing the underlying problem. They were supplementing a tear film whose oil layer was evaporating faster than the drops could replace the water.
Why Calgary specifically
Three environmental factors stack in Alberta in a way that few other Canadian cities match.
The first is humidity. At 30 percent indoor humidity, tear evaporation from the ocular surface increases measurably compared to the 45 to 55 percent range where human tear films evolved to operate. Calgary homes in January routinely sit in the high teens without added humidification.
The second is wind and elevation. Chinook winds are dry and persistent. Elevation thins the atmosphere, increases UV exposure, and accelerates evaporation. Sunglasses help, indoor humidification helps more, and the combination is rarely deployed consistently.
The third is screen behaviour. Blink rate drops by about 50 percent during focused screen work, from roughly 15 per minute to 7 or 8. Incomplete blinks — not fully closing the upper lid — become more common after hours of screen use and further starve the meibomian glands of the mechanical squeeze they need to secrete oil. Every hour of screen time in a dry, heated Calgary office is an hour of cumulative lipid-layer degradation.
Meibomian gland dysfunction: the root cause most patients never hear about
When the lipid layer is the problem, the underlying structural issue is usually meibomian gland dysfunction (MGD). The oil glands along the lid margin become clogged, inflamed, or physically shortened. Untreated MGD is progressive: clogged glands that are not cleared over months and years can atrophy permanently. Meibography — an imaging technique an optometrist uses to photograph the glands — often shows Calgary patients in their 40s with gland loss that should not appear until their 60s.
Treating MGD is a multi-step process that artificial tears cannot replicate. It typically combines lid hygiene, warm compresses or in-office thermal treatment, expression of the blocked glands, and — for more advanced cases — anti-inflammatory drops, oral omega-3 supplementation at therapeutic doses, and in-office treatments such as intense pulsed light (IPL) or thermal pulsation.
The timeline matters. A six-week program with consistent daily lid hygiene and two or three in-office sessions will almost always outperform a year of sporadic drops. The patients who respond best are those who commit to the daily work; the patients who don’t see change are almost always skipping the home component.
What a structured dry-eye workup looks like
A proper dry-eye assessment is not a standard eye exam. It includes a symptom questionnaire calibrated to clinical severity, a tear-film breakup time measurement, osmolarity testing where available, meibomian gland imaging, and an assessment of ocular surface staining with dyes that reveal damage invisible to the naked eye.
- Symptom score using OSDI or SPEED questionnaires to establish a baseline and track change over time.
- Tear breakup time (TBUT), which measures how long the tear film holds together between blinks.
- Meibography to photograph gland structure and flag atrophy early.
- Osmolarity, a number that correlates with disease severity better than symptoms alone.
- Ocular-surface staining to identify dry-spot patterns that drops are not reaching.
- Blink rate and completeness assessment, usually with video, to catch the screen-driven component.
The results usually reveal a specific sub-type — evaporative, aqueous-deficient, or mixed — and a severity grade. Treatment is calibrated to both. Treating every patient with the same lid-hygiene-plus-drops protocol is why most over-the-counter attempts fail.
What the home routine should actually include
Patients who succeed with dry eye usually follow a narrow, daily, ten-minute routine. The content changes with severity, but the outline is consistent.
Start with a warm compress — a commercial eye mask heated to roughly 40°C, held on closed eyes for ten minutes. Follow with a lid wipe using a product formulated for the eyelid margin. Instill any prescribed anti-inflammatory or lubricant drops at the schedule the optometrist sets. Add a daily fish-oil supplement at a dose that delivers at least 1,000 mg of combined EPA and DHA. Address the environment: a humidifier in the bedroom, deliberate breaks from screen use using the 20-20-20 rule, and wraparound sunglasses outdoors.
Patients who adhere to this routine for six to eight weeks typically see meaningful improvement. A Calgary optometry and dry-eye clinic that combines in-office procedures with daily home protocols will usually move a moderate dry-eye patient from daily symptoms to weekly flare-ups over one treatment block.
Contact lens wearers and the Calgary climate
Contact lens intolerance is often the first sign of early dry eye, and many Calgary wearers attribute it to the lens rather than the ocular surface underneath. The typical story: years of comfortable wear, then a gradual decline through the 30s or early 40s with lenses that seem to dry out in the afternoon, feel gritty by evening, and blur between blinks.
The underlying issue is almost always the tear film, not the lens. A lens sits on the tear film, and a degraded film cannot support the lens through a full day. Switching brands rarely helps; the new lens fails the same way within weeks. What helps is treating the dry eye first, then refitting the lens to a material and wear schedule the ocular surface can actually support.
Daily-disposable silicone-hydrogel lenses, scleral lenses for moderate to severe cases, and shorter wear schedules combined with glasses on the worst days are all tools in the fit. The decision is individual, and a proper contact-lens evaluation in the context of a dry-eye workup is the difference between a patient who returns to comfortable wear and one who quietly gives up on contacts entirely.
The long view
Dry eye in Calgary is not a nuisance to manage with drops. It is a progressive disease of the ocular surface driven by a climate that actively degrades the tear film, and it responds to structured care the same way any chronic condition does — imperfectly at first, then more durably as the protocol compounds.
The patients who do best treat dry eye as an ongoing part of their health routine, not an occasional purchase in the pharmacy aisle. The ones who struggle are usually the ones who have been told their eyes are fine, handed a sample of artificial tears, and left to manage the symptoms alone for years. A proper workup reframes the problem, and for patients who want all-inclusive care access in Calgary — vision, primary care, and allied health under one roof — a proper routine holds the result
About the author — this article was contributed by Primaris Health, a Calgary clinic offering integrated vision care — including comprehensive eye exams, dry-eye assessment and treatment, contact-lens fitting, and dermatology support — alongside primary care and allied health services under one roof.